What is an acquired brain injury?
Acquired Brain Injury
TYPE 1
Traumatic Brain Injury (TBI)
- Falls/Trips
- Road traffic accidents
- Extreme sports injuries
- Climbing accident
- Sporting head injuries
- Concussion
- Assault
TYPE 2
Non Traumatic Brain Injury (NTBI)
- Brain Haemorrhage
- Brain Tumour
- Encephalitis
- Meningitis
- Cardiac Arrest
- Drowning
- Suffocation
- Strangulation
- Poisoning/Sepsis
- Chemotherapy
- Covid 19
An acquired brain injury is any damage to the brain that occurs after birth. They are caused by ‘major trauma’ events.
Major trauma describes isolated or multiple serious injuries, that may result in death or disability.
Common causes include:
- Road incidents
- Falls
- Sporting Injuries/Concussions and
- Acts of violence/assault
(Source: South Tees Hospital’s Trust)
Road traffic accidents are the most common cause of ABI in older children and adolescents, whilst falls, being dropped or non-accidental injuries are more common in younger children and infants. (Ref: West, J; Cerebra; 2010)
“The NHS’s Draft Service Specification for Paediatric Neuro-rehabilitation, published in December 2012, estimated that around 40,000 children in the UK suffer a brain injury each Year” This is only an estimated figure and the incidence of acquired brain injury may in fact be much higher.
Of these, approximately:
- 2,000 will have sustained severe traumatic brain injury
- 3,000 moderate traumatic brain injury and
- 30,000 mild traumatic brain injury
However the severity of the brain injury, does not always reflect the level of impairment. In other words a person with a mild head injury may have been more significant impairments than a person with a severe head injury. Each case in unique to the individual.
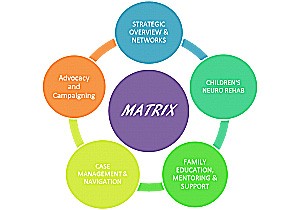 MATRIX Neurological has therefore been formed to enable children and young people who have sustained an acquired brain injury, before the age of 19, to have immediate access upon discharge to high quality community-based services and support tailored specifically to their individual needs. We know our services are currently not available nationally. People supported by us will continue to have access to services from MATRIX Neurological until they are 25.
MATRIX Neurological has therefore been formed to enable children and young people who have sustained an acquired brain injury, before the age of 19, to have immediate access upon discharge to high quality community-based services and support tailored specifically to their individual needs. We know our services are currently not available nationally. People supported by us will continue to have access to services from MATRIX Neurological until they are 25.
ABI is often referred to as a ‘hidden disability’, as survivors may have no physical evidence of their injury. Many of the impairments are not visible to others and it is only over time that the longer term effects may become apparent. The negative consequences of ABI can severely and permanently change a child’s life, as well as have a profound impact on the child’s family as a whole.
Impact on the child:
ABI can cause a range of long term disabilities such as communication and cognitive deficits, sleep disturbance, physical impairments such as post-traumatic epilepsy, depression and high rates of behaviour problems. The more severe the ABI, the greater the impairments of neuro-behavioural functions.
It is usually the cognitive, behavioural and personality changes that produce the greatest disruption to their quality of life. However, the long term effects often arise when children move into adolescence and adulthood and the true extent of these impairments may only become apparent when the child or adolescent returns to education and fails to meet developmental milestones.
Impact on the family:
It is well recognised that ABI affects both the injured individual and the family as a whole. Families experience panic and fear; shock and denial; anger; guilt and isolation and often no hope for the future. Although they eventually adapt to the increased demands of the brain injured child, it is also common for parents of children with an ABI to experience:
- high levels of parental burden and stress
- psychological distress and reduced coping abilities
- deteriorating family relationships and family conflict which often contributes to marital breakdown
- where families also have low social resources or support, the impacts are further exacerbated
(Middleton, JA (2001); Brain Injury in children and adolescents: Advances in Psychiatric Treatment, 7, p257-265)
MATRIX Neurological was primarily set up to work with children, young people and their families who are living with the effects of an acquired brain injury who are in need of help or support. We are aware of the difficulties faced by parents and other community professionals in understanding what has happened and the effects of brain injury on the child or young person. Our services also aim to help parents understand a new way of living and we advocate for the on-going rehabilitation needs of the child or young person across a range of agencies.






